
HOW TO DEAL WITH PSORIASIS & NATURAL REMEDIES FOR IT
What is psoriasis?
Psoriasis is a chronic autoimmune condition. It causes the rapid buildup of skin cells, which creates scaling on the skin’s surface.
BM7 may help with inflammation, skin allergy, Eczema, Dermatitis, Pimples, Acne, Warts, Psoriasis, Urticaria, and many other skin ailments.
Redness and Inflammation around the scales are reasonably common. Psoriatic scales are whitish-silver and develop in thick, red patches. that can crack and bleed.
Normal skin cells grow deep in the skin and slowly rise to the surface. Skin cells don’t last very long, only about three weeks or so. Psoriasis is the result of a sped-up skin production process.
People who have psoriasis experience a build-up of skin cells because of this speedy production process which doesn’t give the skin cells time to fall off before they are replaced. Instead of taking almost a month, this entire process might occur in just a few days. The buildup of skin cells causes scales to develop in areas such as joints, elbows, and knees.
Scales can develop anywhere on the body:
- hands
- feet
- neck
- scalp
- face
(Nails, mouth, and the genital area are much less common).
About 7.4 million Americans have psoriasis. Many of these individuals suffer from other conditions, such as:
BM10 may help your body deal with glycosuria, blood sugar, thirst, and negative feelings.
BM17 may help with anxiety, poor self-confidence, nervousness, fear, tension, sleeplessness, violent palpitation, and impaired memory with hallucinations.
What are the different types of psoriasis?
There are five types of psoriasis:
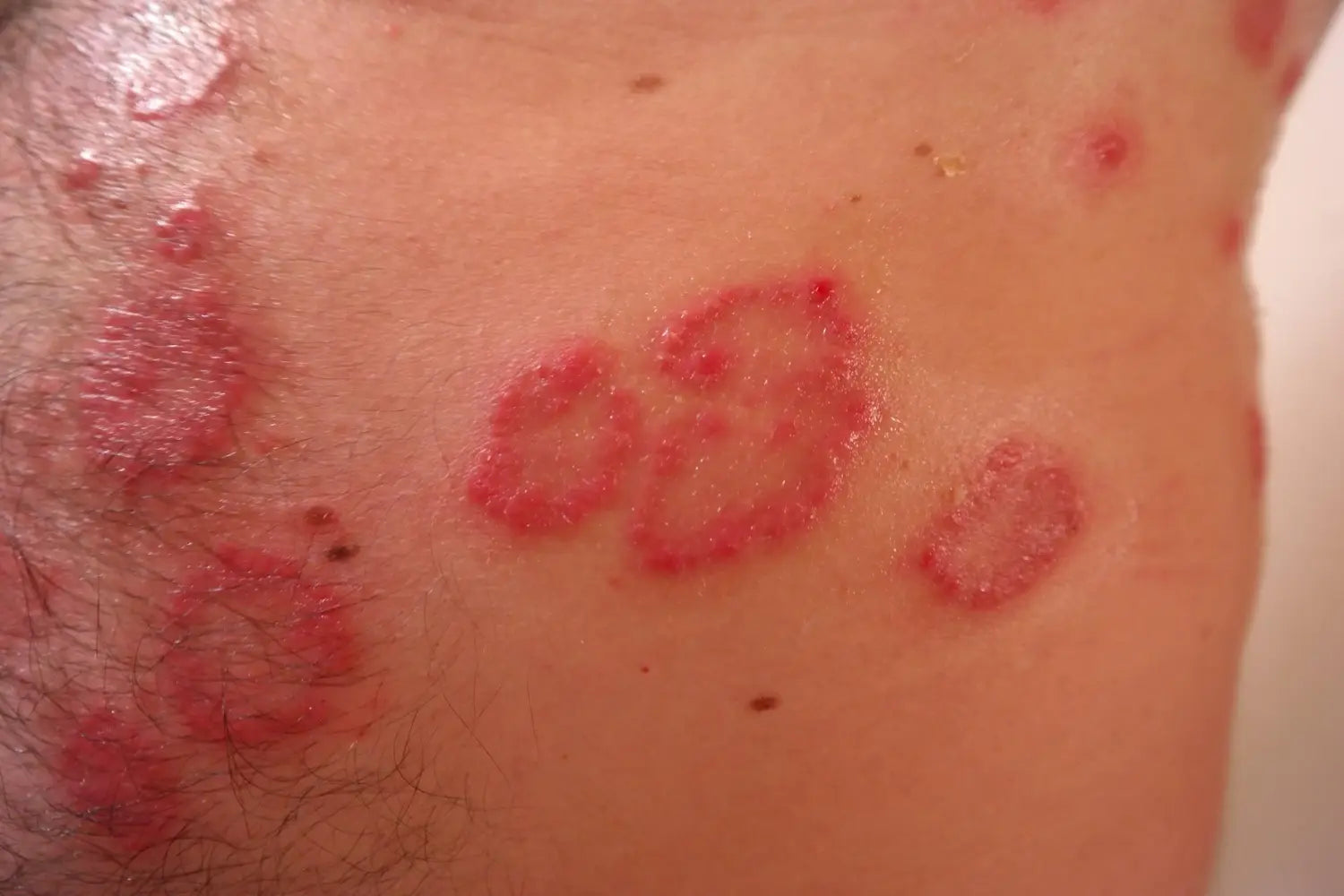
1) Plaque psoriasis
This is the most common type of psoriasis. It causes red, inflamed patches that cover specific areas of the skin with whitish silver scales. Inflamed skin plaque is most often found on the knees, elbows, and scalp. About 80% of people with psoriasis have plaque psoriasis according to the American Academy of Dermatology.
2) Guttate psoriasis
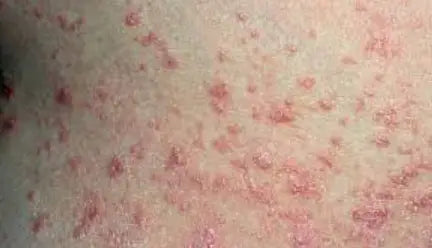
Children are most likely to develop this type of psoriasis. Guttate causes a rash with small pink dots, but the thick raised scales of plaque psoriasis are notably absent. The most common sites for guttate psoriasis include the torso, arms, and legs.
3) Pustular psoriasis
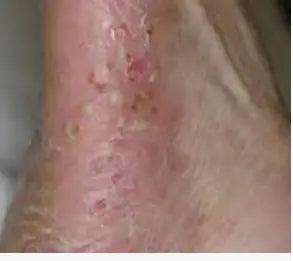
This form is more common in adults. Usually, it affects smaller areas of the body like the hands, but now and then it becomes a more widespread condition. The symptoms vary with the different types of psoriasis, in the cases of pustular psoriasis it causes white, pus-filled blisters and areas of red, inflamed skin.
4) Inverse psoriasis
Shiny, red,, and inflamed skin are all common symptoms of Inverse psoriasis. Patches of affected skin may develop under armpits or breasts, in the groin, or around the genitals.
5) Erythrodermic psoriasis
Erythrodermic psoriasis is a very serious and rare type of psoriasis.
It can cover large sections of the body. The skin might look sunburned. Scales that develop often peel off in large sections. Fevers and illness are commonly associated with this type of psoriasis. In some cases,, the illness can even become life-threatening. A doctor should consult to ensure your health and safety if you suffer from Erythrodermic psoriasis.
Kali Sulph is best used for eruptions on the skin and scalp problems, especially when there is yellow pus. It may help carry oxygen to your cells and benefit respiration. Useful when you feel stuffed up or have a cough with yellow phlegm & more.
Symptoms
Psoriasis causes a buildup of skin cells on the skin’s surface, which leads to scaly patches of skin.
If you have pale skin psoriasis will usually appear as pink or red patches with silvery white scales. With a darker complexion, psoriasis is more likely to appear as purple or brown patches with gray scales.
Psoriasis can go into remission and leave you symptom-free, the average length of remission is 1 to 12 months. Flare-ups can cause intense symptoms which eventually subside into another period of remission. The cycle of flares ups and remission can be difficult to predict and hard to control.
Symptoms can present as anything from mildly irritating to severely painful lesions; they may also present differently according to the type of psoriasis.
- Mild psoriasis covers less than 3% of the body.
- Moderate psoriasis covers 3–10% of the body.
- Severe psoriasis covers more than 10% of the body.
- the National Psoriasis Foundation
Plaques can develop anywhere, but they commonly occur as small patches on the elbows, knees, lower back, and scalp.
Causes and triggers
Psoriasis is considered an autoimmune condition, but the cause is currently unknown. Autoimmune conditions affect the immune system, which produces T cells that are designed to protect your body from infection.Psoriasis triggers such as infections, weather,, or injury can lead to genes instructing the immune system to target the wrong cells. T cells respond the same to a trigger as they would to an actual infection or injury. This process causes inflammation.
In psoriasis, this autoimmune system shifts into overdrive and this leads to the excessive growth of skin cells. Typically, skin cells take about 1 month to replace themselves. In people with psoriasis,, a measly 3–4 days completes this process.
Not everyone’s triggers are the same, some common triggers are:
- hormonal imbalances
- depression stress and anxiety
- skin injuries
- infections
- lithium
- beta blockers
- antimalarials
- quinine
- interferons
- indomethacin
- (NSAIDs)non-steroidal anti-inflammatory drugs
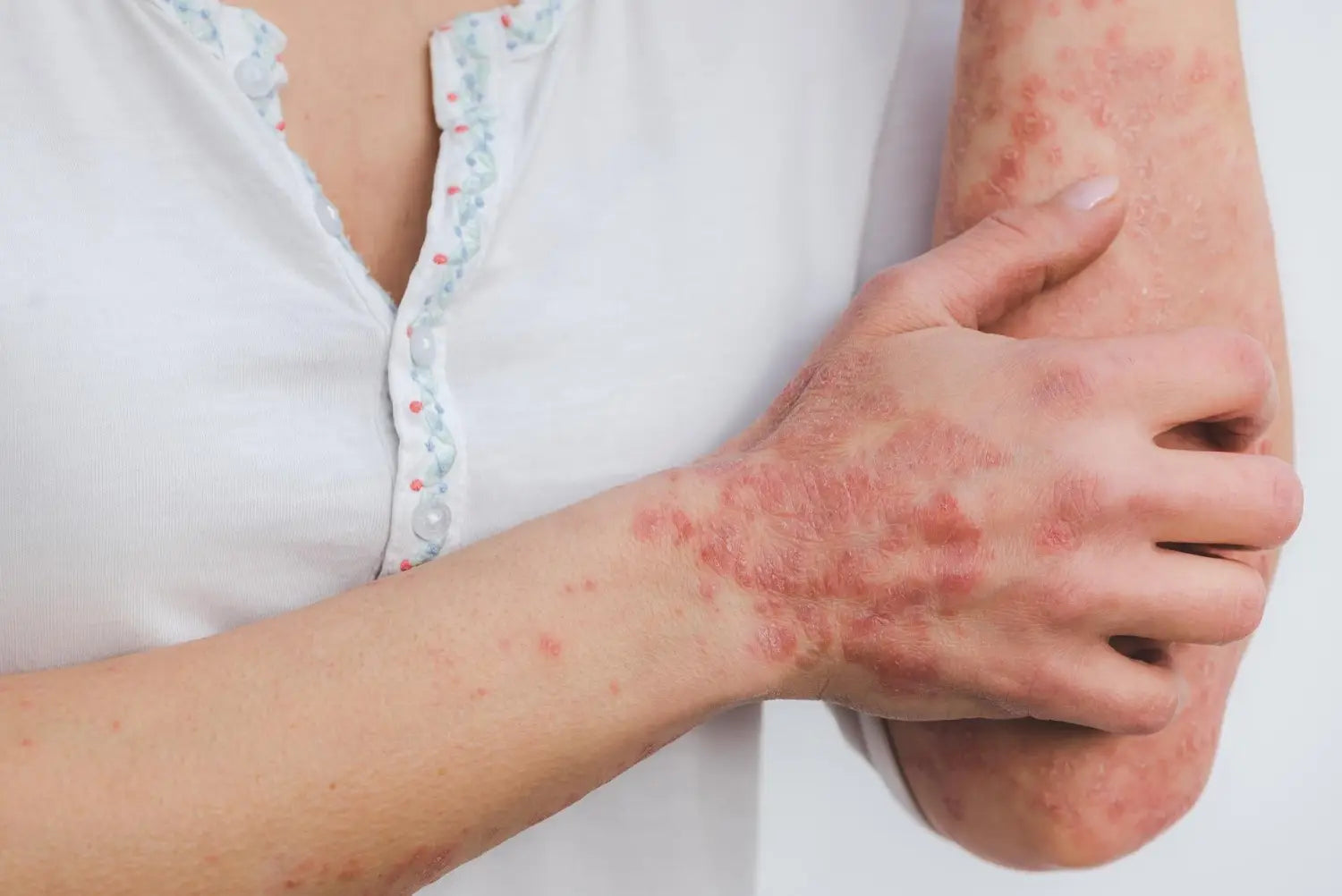
Risk factors
There are a variety of factors that can increase the risk of a person developing psoriasis.- obesity
- family history
- cardiovascular disease
- metabolic syndrome
- trauma to the skin
- hypertension
- diabetes
- infection
- obesity
Studies have found more than 60 genetic markers that are linked to Th17 cell activation. This is the primary element that causes inflammation in psoriasis. Genetics is an important factor that can help determine how at-risk someone is for developing psoriasis. About 40% of people with psoriasis or psoriatic arthritis have a family history of the condition.
Infections like strep throat, bronchitis, and tonsillitis can cause psoriasis to flare up especially if the person experiencing the illness is young.
Gender doesn’t make a difference when it comes to psoriasis, it is equally unpleasant for males and females. Onset is most common between the ages of 15 and 25 years. About ⅓ of people that suffer from psoriasis have had it since they were kids.
BIO20 supports healthy cell regeneration and promotes the skin's youth, radiance, and healthy appearance. This combination of cell salts is useful for eczema, psoriasis, acne, pemphigus, and dandruff. It is also useful for visible scars, cradle caps, and neonatal dermatitis.
Is psoriasis contagious?
Psoriasis isn’t contagious. You can’t pass the skin condition from one person to another. Touching a psoriatic lesion on another person won’t cause you to develop the condition.
It’s important to be educated on the condition, as many people think psoriasis is contagious.
Diagnosing psoriasis
Sometimes psoriasis can be confused with other skin conditions depending on how the symptoms present. When the psoriasis plaque forms in specific areas of the body it is easy to tell. If it is not so easy to tell the doctor might want to do some further testing.
Physical examination
Most doctors can make a diagnosis with a simple physical exam. Symptoms of psoriasis are most often easy to distinguish from other conditions that may cause similar symptoms.
During this exam, be sure to show your doctor all areas of concern. In addition, let your doctor know if any family members have the condition.
Biopsy
If the symptoms are unclear or if your doctor wants to confirm their suspected diagnosis, they may take a small sample of skin. This is known as a biopsy.
The skin will be sent to a lab, where it’ll be examined under a microscope. The examination can diagnose the type of psoriasis you have. It can also rule out other possible disorders or infections.
Most biopsies are done in your doctor’s office the day of your appointment. Your doctor will likely inject a local numbing medication to make the biopsy less painful. They will then send the biopsy to a lab for analysis.
When the results return, your doctor may request an appointment to discuss the findings and treatment options with you.
Treatments
If a doctor confirms that a person has psoriasis, treatment will depend on the variety and severity of the condition. The most common types of treatment are medication and phototherapy.
Emollients are useful for keeping the skin moisturized while you are using other healing treatments to help with the underlying cause, the response of your body’s immune system. Proper moisture levels will help decrease the itching and irritation too. A reduction in the number of lesions and plaque formation may also result from continued use.
Medications
Topical, oral, and injected medications are all available treatment options for people with psoriasis.
Topical therapies
People apply topical treatments directly to the skin. This option is usually the first-line treatment for mild-to-moderate symptoms, and it aims to slow down the growth of skin cells, reduce inflammation, and soothe itching or discomfort.
Over-the-counter (OTC) remedies may relieve the mild symptoms of psoriasis. Here are some examples:- Coal tar helps soothe plaque psoriasis, itching, and lesions on the scalp, palms, and soles. Can be used on its own or combined with another type of treatment.
- Hydrocortisone creams can reduce inflammation and soothe itching.
- Salicylic acid reduces swelling and helps remove scales, a great option
From the Doctor...
- Corticosteroids: Doctors often recommend corticosteroids to help treat psoriasis symptoms. Steroids are available as gels, foams, creams, sprays, and ointments. Click here to go to the National Psoriasis Foundation where you will find a guide to help you understand corticosteroid treatments and other options
- Synthetic vitamin D: People often use this in conjunction with corticosteroid cream or ointment. It promotes slower skin cell growth, flattens plaque formations, and diminishes scale growth.
- Retinoid Creams and Gels: Synthetic vitamin A (eg. Tazarotene) is also able to slow the overgrowth of skin cells, reduce itchiness and minimize skin discoloration. WARNING retinoids can also irritate the skin causing burning and stinging, peeling, and pain.
- Immunomodulators: Pimecrolimus cream and tacrolimus ointment are non-steroidal and help suppress the immune response that causes psoriasis. A doctor may prescribe them to help reduce the symptoms of inverse and plaque psoriasis. People often combine them with a course of steroids.
BM39 is best used for mastocytosis (numerous, itchy, irregular, yellow or orange-brown swelling on the skin); allergy from food (milk, eggs, shellfish or nuts); and medicine allergy.
Systemic therapies
Designed for people who have moderate to severe psoriasis and psoriatic arthritis, systemic therapies work throughout the systems in your body. They help diminish disease progression and prevent the recurrence of flares.
For more information about systemic therapies keep reading….details are coming up.
Biologics
Drugs that have a protein base and are derived from living cells are called biologics. They target the T cells and immune proteins that cause psoriasis and psoriatic arthritis.
The Food and Drug Administration (FDA) has approved multiple biologics. These include etanercept, infliximab, and adalimumab. While the FDA may have approved them you have to consider the potential side effects of all 3 of these medications before you decide what the right course of treatment is for you.
Possible side effects….
- sinus congestion and runny nose
- sore throat with fever and chills
- headaches
- rash
- stomach pain
- muscle /bone pain
Methotrexate
Doctors prescribe methotrexate for extremely severe psoriasis that restricts daily function and does not respond well to any other treatments. Methotrexate is effective for psoriatic arthritis, as well as erythrodermic, palmoplantar, and nail psoriasis. Extreme types of psoriasis can interfere with your plans and decrease your quality of life, but the side effects of this drug are not exactly pleasant so you need to decide if this is the right option for you.And the side effects are …
- drowsiness
- dizziness
- headaches
- hair loss ( isn’t that great , because you weren’t self conscious enough about your psoriasis)
- decrease in normal appetite level
- red eyes
Cyclosporine
Normally doctors would prescribe cyclosporine for preventing the rejection of organs after transplants. Preventing organ rejection is “hugely” imporant. People might be willing to put up with any number of side effects in order to continue living with a new and functional organ. However, when used for people with severe presentations of plaque, generalized pustular, guttate and erythrodermic psoriasis the side effects might cause a different level of concern. Each person needs to weigh the pro’s and con’s of their own situation.To make sure your decision is a good one, you need to know what could happen if you take this particular drug…
- inflamed and swollen gums
- high blood pressure
- tingling and numbness in your extremities
- increased/unwanted hair growth
And if that wasn’t enough it can cause tremors, stomach upset, diarhea, headaches and changes in blood sugar.
Oral retinoids
Oral retinoids do not decrease the immune response in the body making it a great option for those with severe psoriasis that also have a suppressed immune system. Such as people with HIV or some other autoimmune disorder. Acitretin, works against the effects of the condition throughout the body.
People with all types of psoriasis except inverse psoriasis may benefit from using oral retinoids.Yet I am still going to issue a word of warning, the Mayo clinic has a list of side effects categorized as more common, less common, rare, and incidence unknown, It is a very long and comprehensive (and somewhat scary) list check it out for your self.
Off-label medications
Doctors may prescribe certain off-label medications if the standard FDA-approved drugs have not resolved a person’s symptoms or if the individual has another condition that prevents the use of specific medications.
However, due to several safe biologics recently coming to market, this is now a less common approach.
Phototherapy
Phototherapy, also known as light therapy, is the use of ultraviolet light for its healing effects. the skin is regularly exposed to certain lights and lasers under medical supervision. The light can slow cell growth, suppress immune activity, and reduce irritation.
DIY options are available, people can carry out phototherapy at home using a lightbox or handheld device if their initial treatment is successful. Lots of affordable options can be found online. Prices can be as low as $50 and as high as $500, do your research to make sure you are getting the best product possible. Some people may also need to take psoralen pills before exposure to make their skin more sensitive to light.
Anyone who has coexisting conditions that make them sensitive to light, such as lupus or previous instances of skin cancer, should not use phototherapy.

Home remedies
Completely avoiding psoriasis flares is impossible. However, a person may be able to reduce their risk of flares with some simple and effective lifestyle changes. These strategies can work alongside traditional treatment plans.Some strategies include:
- reducing stress with yoga, exercise, and meditation
- eating a balanced diet
- recognizing and avoiding food triggers (you might want to keep a food journal for this one)
- not smoking or drinking alcohol in excess
Unfortunately, psoriasis can be isolating and uncomfortable. The good news is people have a lot of options for managing the symptoms and limiting the immune activity related to the condition.
Homeopathy & Psoriasis
Homeopathy can help stimulate the body’s natural healing and help restore natural immune system response and function. Psoriasis of the skin responds very well to homeopathic remedies. Psoriatic arthritis and psoriasis of the scalp and nails can be more difficult to treat.
Remedies that have proven to be an effective treatment for psoriasis:
- arsenic album - use for silver scales
- merc sol - use for scalp psoriasis
- graphites naturalis - use for cracked skin
- sepia succus - for oval lesions
- arsenic iodatum - use for shedding of large scales caused by psoriasis
- petroleum oleum- use for deep cracks
- sulphur - use for intense itching and burning
Remedies will not cause side effects and may be used on their own or combined with your current treatment to provide you with optimal relief.
Psoriasis diet
Psoriasis cannot be cured by what you eat, but the National Psoriasis Foundation believes eating a healthy diet may help a person with psoriasis minimize their symptoms and reduce the risk of developing certain complications.Inflammation is a main symptom of psoriasis. Certain food choices can help reduce or even prevent inflammation in the body. Maintaining a healthy diet may also reduce the risk of developing complications such as diabetes, high blood pressure, and heart disease.
The National Psoriasis Foundation recommends that people with the condition eat a varied, healthy diet that includes:
- limiting alcohol intake
- prioritizing lean protein sources, such as chicken breast
- eating fish rich in omega-3 fatty acids
- reducing gluten intake, if a person has a gluten allergy
- avoiding pro-inflammatory foods, such as simple carbohydrates and saturated fats
Bottom line
The root cause of psoriasis is unclear. Environmental triggers including stress, hormonal changes, cleaning products and more — can all cause symptom flares.
Recent developments in treating psoriasis have led to a reduction in the number of flares and the severity of flares most people experience. this is not a cure but it is a step in the right direction.
Treatments for mild cases of psoriasis include topical ointments and lifestyle adjustments. However, in severe cases, rheumatologists may prescribe more advanced treatments, such as corticosteroids, retinoids, biologics, or phototherapy.
In the end the decision is up to you regarding how to treat your psoriasis. Based on how serious your skin condition is and how resistant it has been to treatment you can decide to add, remove or completely change your current treatment plan. Always know your options and keep your doctor informed!









Leave a comment