
WHAT IS ANEMIA? SYMPTOMS AND TREATMENT OPTIONS.
WHAT IS ANEMIA?
Anemia is “the condition marked by a deficiency of red blood cells or of hemoglobin in the blood.” Hemoglobin is an iron-rich protein that gives your blood its red color. It helps cells bring oxygen from your lungs to the rest of your body.
If you have anemia, your body simply doesn’t receive enough oxygen-rich blood, leaving you tired and weak. Red blood cells contain hemoglobin. They are also important for immunity, including fighting infections, as well as clotting blood and preventing too much bleeding.
Anemia is closely related to iron deficiency. According to the Centers for Disease Control and Prevention (CDC), iron deficiency is the most common nutritional deficiency in the U.S. Iron helps produce hemoglobin, and therefore the CDC estimates that almost 10 percent of women are iron-deficient.
This is alarming considering the essential roles that iron plays, including facilitating with oxygen distribution. Your body needs iron to perform many functions throughout every single day. But it’s common for many people to live with low iron levels due to factors like blood loss (such as from menstruation), a poor diet or an inability to absorb enough iron from food sources.
Nat Mur is best used for any dryness or wetness on the body. It may help with diarrhea, runny nose, vomiting, dry, painful throat, and more. Useful for weight loss, delayed menstruation, coldness, dyspepsia, eczema, neuralgia, and anemic patients.
Types of Anemia
Haemorrhage: After accidental trauma, heavy bleeding during periods in women or bleeding during childbirth, bleeding in medical conditions like gastric ulcers, inflammatory bowel disease, cancer of gut, parasitic infestation in gut-like hookworm, Schistosomiasis.
Iron deficiency: Iron Deficiency Anemia is common during pregnancy and lactation and from acute haemorrhage or chronic blood loss. The cause is either a decreased intake of iron rich diet or impaired absorption of iron in the gut.
Deficiency of Vitamin B12 or Folic Acid: It leads to Megaloblastic Anemia.
Pernicious Anemia: This type of Anemia arises from an autoimmune disorder where there is atrophy of gastric mucosa with the resultant decrease in parietal cells and intrinsic factor produced by these cells. Intrinsic factor is required to absorb Vitamin B12. So, in Pernicious Anemia, defective absorption of Vitamin B12 is the cause and not its nutritional deficiency.
Haemolytic Anemia: It is a result of destruction of red blood cells as in malaria, and abnormal red blood cells prone to breakage as in Sickle Cell Anemia.
Thalassemia: An inherited disorder in which the haemoglobin production is impaired.
Symptoms of Anemia:
Pallor; weakness or fatigue; vertigo; mouth soreness; difficulty in breathing or shortness of breath; palpitation; jaundice in Haemolytic Anemia; Koilonychia (spoon-shaped nails) in Iron Deficiency Anemia; pica (desire to eat strange indigestible things including chalk, clay, lime, dry rice, etc) in Iron Deficiency Anemia; gastric symptoms (like diarrhoea, nausea and vomiting); tingling and numbness of limbs in Pernicious Anemia.
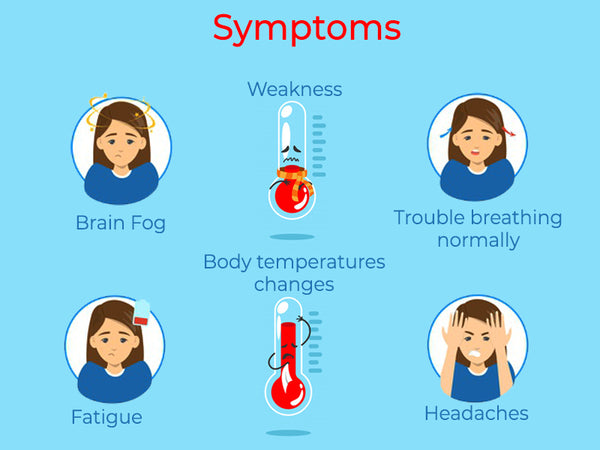
Without enough oxygen-carrying red blood cells in your body, it’s impossible to transport adequate amounts of oxygen to your brain, tissues, muscles and cells. Feeling a little “out of it” and tired is pretty common for many adults, due to compounding reasons. These can include stress, lack of sleep, battling a virus and a busy work schedule, among others. Therefore, when it comes to knowing whether or not you should be checked for anemia, it’s important to understand how anemia symptoms usually manifest and what makes them different than simply feeling exhausted due to other life circumstances.
Here are some of the most common anemia symptoms adults tend to experience:
- Fatigue
- Weakness
- Pale skin
- A fast or irregular heartbeat
- Shortness of breath, trouble breathing, low stamina and reduced endurance
- Chest pains
- Dizziness or loss of stability
- Cognitive problems, including brain fog, difficulty concentrating and trouble getting work done
- Cold hands and feet or other signs of body temperature changes
- Headaches
BM41 may help with of appetite loss, nausea, vomiting, decreased urination, puffy face, weight loss, paleness, and poor nutrient absorption.
You should also be aware that, initially, anemia can be so mild that it often goes unnoticed for a period of time, sometimes even for years. But anemia symptoms typically worsen as the condition progresses, especially if more than one risk factor is contributing to the problem.
There are three primary reasons why you might develop anemia from not having enough red blood cells:
- You’re not producing enough red blood cells.
- You’ve been losing too much blood due to injury, menstruation or other circumstances that cause bleeding.
- Your body is destroying the red blood cells you have due to changes in your immune system.
Anemia can significantly affect a patient's ability to carry on even normal activities of daily living. Therefore, approaches--including the treatment of - drug therapies, even some surgical procedures, complementary and alternative options (herbal, homeopathic, nutritional supplements eg. b12, vit.c), good diet, would be expected to improve quality of life.
BM208 is recommended for iron absorption, extreme fatigue, and skin pallor.
TREATMENT OPTIONS
Although you might be able to treat anemia on your own by making changes to your diet, lifestyle and the supplements you take, it’s also a good idea to talk with your doctor if you suspect you have anemia, considering it can be a side effect of other serious illnesses. You might be exhausted and finding it hard to concentrate for other reasons that have nothing to do with anemia. So, don’t necessarily assume you’ve diagnosed yourself accurately. If anemia symptoms persist after you’ve made the food changes, be sure to get tested for nutrient deficiencies and get a doctor’s opinion.
Anemia treatment options
Anemia treatment can include everything from dietary supplements to blood transfusions. In some cases, a doctor might also use supplementary treatments like intravenous fluids and pain relievers to deal with pain and prevent complications.Anemia medications
Erythropoiesis-stimulating agents (ESAs)
Erythropoietin (EPO) is a hormone produced by the kidneys and helps catalyze red blood cell production. It also promotes blood cell synthesis with hemoglobin, which allows the cells to carry oxygen throughout the body. An erythropoietin shortage is one of the causes of anemia, and EPO-stimulating drugs like Procrit and Epogen can help the body generate more essential red blood cells. These drugs are effective for a variety of anemia cases, but side effects can include hypertension, headaches, body aches, nausea, and vomiting.
Iron supplements (ferrous sulfate)
These supplements replenish the body's iron levels, enabling it to continue producing adequate red blood cells and hemoglobin. According to UCSF Health, an adult male body stores 1,000 mg in iron, and an adult female has 300 mg. Generally, iron should come from a healthy, well-rounded diet, but blood loss from menstrual bleeding, gastrointestinal bleeding, or acute injury can quickly deplete these stores. That’s where iron supplements like Feosol and Slow FE come in. They’re best absorbed on an empty stomach or with vitamin C from a glass of orange juice. Unlike other vitamins and minerals in the body, it's possible to overdose on iron, so carefully follow a doctor's recommendation and the dosage guidelines.
Vitamin B supplements
Vitamin-deficiency anemia often requires vitamin B-12 or folate (vitamin B-9) supplements, which are available over the counter at pharmacies and health food stores. By replenishing vitamin levels, they allow the body to resume normal blood cell production. Some anemia patients only require supplements for a short period of time, while others take them for life—it all depends on the anemia’s cause and severity. Side effects are rare but may include headache, dizziness, nausea, and vomiting.
What are some common side effects of anemia medication?
Every anemia medication has a small chance of side effects. Iron pills have the potential side effect of upset stomach and constipation. They can also cause nausea, vomiting, and heartburn.Vitamin B12 supplements can cause nausea and vomiting too, along with dizziness and headache, while folate supplements sometimes prompt bloating, nausea, trouble sleeping, and poor appetite.
Anemia patients that require an erythropoiesis-stimulating agent like Procrit, Epogen, or Aranesp may experience headaches, body aches, nausea, and vomiting.
These are the most common side effects, but this certainly isn't a complete list. It's important to consult a healthcare provider about all potential side effects and drug interactions before beginning a medication or other treatment.

Diet
Diet is important. People are often surprised by the profound impact dietary changes can have on their lives. Sometimes, thoughtful and dedicated diet changes are all that's necessary to treat anemia, primarily for cases associated with minor vitamin deficiencies. For example, people with iron deficiency anemia would want to fortify their diets with iron-rich foods like:
- Dark green, leafy vegetables
- Red meats
- Eggs
- Soy products
- Legumes
- Broccoli
- Fish
- Fish
- Greek yogurt
- Liver
- Eggs
- Milk (both dairy and fortified non-dairy)
- Citrus fruits and juices
- Leafy greens
- Seafood
- Beans
- Peanuts
- Whole grains
A well-balanced diet that includes many of the foods listed above is a great way not just to prevent anemia, but to maintain overall health. Supplements are great, but it's best to obtain iron and vitamins through a natural diet.

Add these foods to your diet to get more iron and help fight iron deficiency anemia:
1. Leafy greens
Leafy greens, especially dark ones, are among the best sources of nonheme iron. They include:- spinach
- kale
- collard greens
- dandelion greens
- Swiss chard
Some leafy greens such as Swiss chard and collard greens also contain folate. A diet low in folate may cause folate deficiency anemia. Citrus fruits, beans, and whole grains are good sources of folate.
When eating dark, leafy greens for iron, there’s a catch. Some greens high in iron, such as spinach and kale, are also high in oxalates. Oxalates can bind with iron, preventing the absorption of nonheme iron.
So while it’s beneficial to eat your greens as part of an overall anemia diet, don’t depend on them solely to treat the condition.
Vitamin C helps your stomach absorb iron. Eating leafy greens with foods that contain vitamin C such as oranges, red peppers, and strawberries may increase iron absorption. Some greens are good sources of both iron and vitamin C, such as collard greens and Swiss chard.

2. Meat and poultry
All meat and poultry contain heme iron. Red meat, lamb, and venison are the best sources. Poultry and chicken have lower amounts.Eating meat or poultry with nonheme iron foods, such as leafy greens, along with a vitamin C-rich fruit can increase iron absorption.
3. Liver
Many people shy away from organ meats, but they’re a great source of iron.
Liver is arguably the most popular organ meat. It’s rich in iron and folate. Some other iron-rich organ meats are heart, kidney, and beef tongue.
4. Seafood
Some seafood provides heme iron. Shellfish such as oysters, clams, scallops, crabs, and shrimp are good sources. Most fish contain iron.Fish with the best levels of iron include:
- canned or fresh tuna
- mackerel
- mahi mahi
- pompano
- fresh perch
- fresh or canned salmon
Calcium may bind with iron and reduce its absorption. Foods high in calcium shouldn’t be eaten at the same time as iron-rich foods.
Other examples of calcium-rich foods include:
- dairy milk
- fortified plant milks
- yogurt
- kefir
- cheese
- tofu

5. Fortified foods
Many foods are fortified with iron. Add these foods to your diet if you’re a vegetarian or struggle to eat other sources of iron:- fortified orange juice
- fortified ready-to-eat cereals
- foods made from fortified refined flour such as white bread
- fortified pasta
- foods made from fortified cornmeal
- fortified white rice
6. Beans
Beans are good sources of iron for vegetarians and meat eaters alike. They’re also inexpensive and versatile.Some iron-rich options are:
- kidney beans
- chickpeas
- soybeans
- black-eyed peas
- pinto beans
- black beans
- peas
- lima beans

7. Nuts and seeds
Many types of nuts and seeds are good sources of iron. They taste great on their own or sprinkled on salads or yogurt.Some nuts and seeds that contain iron are:
- pumpkin seeds
- cashews
- pistachios
- hemp seeds
- pine nuts
- sunflower seeds
Almonds are also a good source of iron. They’re great as part of a healthy eating plan, but since they’re also high in calcium, they may not increase your iron levels that much.
Takeaway
No single food will cure anemia. But eating an overall healthy diet rich in dark, leafy greens, nuts and seeds, seafood, meat, beans, and vitamin C-rich fruits and vegetables can help you get the iron you need to manage anemia.Be sure to discuss supplements with your healthcare provider because it’s difficult to get enough iron from diet alone.
A cast iron skillet is an anemia diet plan staple. Foods cooked in cast iron absorb iron from the skillet. Acidic foods absorb the most iron, and foods cooked for short periods of time absorb the least.
When following a diet plan for anemia, remember these guidelines:
- Don’t eat iron-rich foods with foods or beverages that block iron absorption. These include coffee or tea, eggs, foods high in oxalates, and foods high in calcium.
- Eat iron-rich foods with vitamin C-rich foods, such as oranges, tomatoes, or strawberries, to improve absorption.
- Eat iron-rich foods with foods that contain beta carotene, such as apricots, red peppers, and beets, to improve absorption.
- Eat a variety of heme and nonheme iron foods throughout the day to up your iron intake.
- Eat heme and nonheme iron foods together whenever possible to increase iron absorption.
- Add foods rich in folate and vitamin B-12 to support red blood cell production.
BIO1 is best used for problems associated with Iron-deficiency. It may support your body in managing, absorbing, and using needed nutrients. Effective natural support for the immune system and energy levels.
Natural Homeopathic Treatment For Anemia
The Homeopathic mode of treatment, with the use of medicines made of natural substances, is very effective in treating Anemia. There are a variety of Homeopathic remedies for Anemia. The medicines are solely selected on the basis of individual symptoms.https://bestmadenaturalproducts.com/products/iron-absorbing-remedy-bm208
CONCLUSION
Whatever treatment you and your doctor decide upon, be sure to follow through to get optimal results.
With better understanding of your condition it’s easier to find the most effective and safest way to help yourself.







Leave a comment